What Are You Looking For?

For 5-year-old Mengmeng, what should have been carefree childhood years were overshadowed by a relentless cycle of chronic cough, rhinitis, otitis, and pharyngitis for nearly three years. Her desperate parents sought medical help, leading to the surgical removal of her enlarged tonsils and adenoids. Yet, relief was temporary, and the distressing symptoms returned.
Their relentless search for answers finally led them to a top-tier hospital in Zhejiang Province, where Mengmeng was accurately diagnosed with pathological gastroesophageal reflux disease (GERD). With targeted medication, her symptoms vanished. The cheerful, healthy child her parents had missed for so long finally re-emerged.
What is Pediatric GERD?
Gastroesophageal Reflux Disease (GERD) in children occurs when stomach contents, including acid and pepsin, flow back into the esophagus and beyond—reaching the throat, mouth, or even lungs. This causes a range of symptoms and complications. The unique physiology of children often leads to misdiagnosis or underdiagnosis of pediatric GERD.
Why Do Children Experience GERD?
In infants under 1 year old, the lower esophageal sphincter is still developing, making spitting up or “physiological reflux” common. This typically resolves by age 1-2.
However, in some children, reflux is severe. The constant irritation of the airways can lead to persistent cough, wheezing, and recurrent infections, signaling a need for medical evaluation.
For children over 2, physiological reflux is rare. Here, GERD is often linked to diet and lifestyle factors like obesity, overeating before bed, irregular meals, and high-fat diets, which strain the stomach and weaken the esophageal sphincter.
What Are the Symptoms of Pediatric GERD?
Key signs include chronic cough, acid regurgitation, heartburn, and chest discomfort. In children, symptoms often manifest as recurrent respiratory issues, making accurate diagnosis crucial.
How is Pediatric GERD Detected?
When a child shows persistent symptoms, especially if they recur after standard treatment, specific testing is essential. Common clinical methods include the PPI trial, barium studies, endoscopy, pH monitoring, and esophageal manometry.
Among these, saliva pepsin testing stands out as the simplest, most non-invasive method, making it exceptionally suitable for children.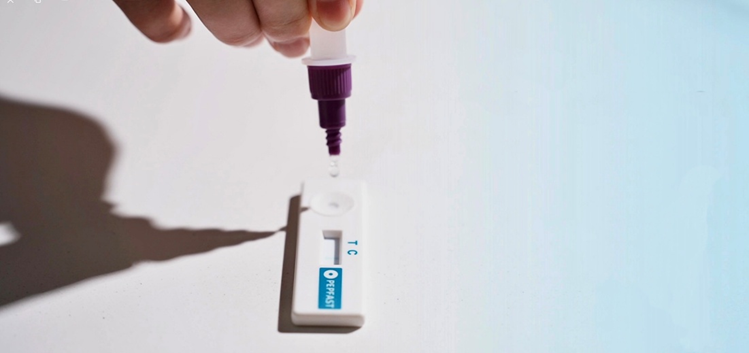
Pepfast, a leading rapid pepsin detection kit, exemplifies this advantage. The test is completely non-invasive: simply collect a small saliva sample one hour after a meal. The process is painless, requires high child compliance, and puts parents at ease. Most importantly, it delivers accurate results within 15 minutes, preventing long waits and allowing for timely clinical decisions. This efficiency has made it a preferred choice for both doctors and families.
Leave A Message